Cardiovascular disease and specifically heart failure is the number one cause of death in people across just about any demographic. If we had a patient with a bad heart and we could take their heart out and replace it with a machine, we’d do it all the time. For the last half-century, scientists have been working tirelessly to create a machine that can accurately mimic the function of a beating human heart, envisioning devices they hope will one day rid us of the number one cause of death in the world.
Every technology goes through a sigmoidal adoption curve. 5% of people are doing it, then 20, then 15, suddenly it saturates and goes vertical. And only now in the last decade or so have we had the technology to make devices that potentially could last a decade or more. If we had a practical, permanent, total artificial heart, it would be one of the biggest accomplishments in modern medicine. When it comes to heart failures, there is currently only one gold standard of treatment: replacing the failing heart with that of a healthy donor. And while there are nearly 6,000 heart transplants done annually, there are about a million requests for donor’s hearts each year, 600,00 of which are in the US alone.
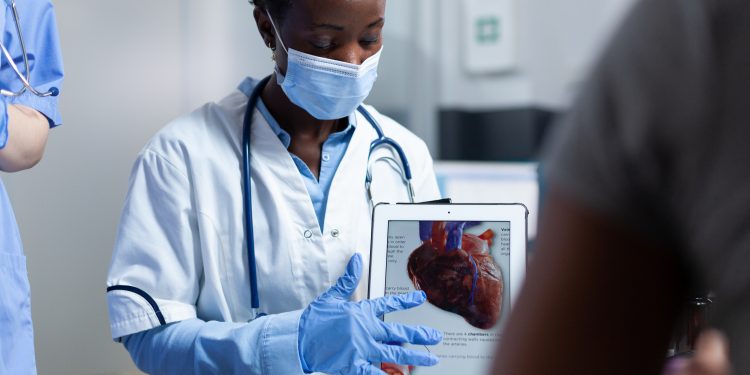
Your heart is just a pump. Every cell in your body needs nutrition, needs oxygen. It gets that through the blood that goes through every blood vessel in your body. The heart is the pump that makes the blood move. So, the heart is a remarkably simple device by some metrics, but incredibly complex by others.
The first artificial heart was designed by a brilliant Argentinian scientist Domingo Liotta who was working at the Cleveland Clinic and then came to work with Michel DeBakey, a pioneering heart surgeon in Houston. They developed a device that DeBakey had implanted in seven cows. The longest went about 12 hours. On April 4th, 1969, was the first clinical use of a total artificial heart. Unfortunately, the valves that they had put in this version of the heart were breaking up the blood, the broken-up blood was causing the kidneys to fail, and after 64 hours (about 2 and a half days) on the device, an emergency transplant had to be done. 36 hours (about 1 and a half days) later the patient died of an infection. But it showed us that this kind of thing was possible.
Based on that technology, that device continued to evolve and evolved into what we now have, the SynCardia device, which is the world’s first approved device, just like the one implanted in 1969, but with much better membranes, much better valves, much better material and manufacturing techniques. Then in 2021, the Carmat device was approved for commercial sale in Europe. SynCardia and Carmat are currently approved only as bridges to transplant devices, temporary hearts that keep patients alive until a real donor heart becomes available. The longest an artificial heart has ever lasted in a patient is 1,374 days or roughly four years, the real limitation being long-term durability.
Bio fabrication of perfect human hearts is a most challenging and more less impossible task. Many studies have reported that artificial hearts have had complications related to the immune response of the system. A recent research study reports a major step forward in fabricating an artificial heart, fit for a human. By recreating the helical structure of heart muscles, researchers improve their understanding of how the heart beats through this study.
Bioengineers have developed the first biohybrid model of human ventricles with helically aligned beating cardiac cells, and have shown that muscle alignment does, in fact, dramatically increase how much blood the ventricle can pump with each contraction. Tissue engineering, ultimately including the wholesale fabrication of an entire human heart for transplant, is so important for the future of cardiac medicine. The study was published in a science journal and researchers from Harvard University, Boston, University of Pittsburgh, USA.
To build somebody’s heart from the ground up, researchers have to replicate the unique structures that structure the heart. But creating hearts with different geometries and alignments has been challenging. Now, bioengineers from Harvard John A. Paulson School of Engineering and Applied Sciences (SEAS) have developed the primary biohybrid model of human ventricles with helically aligned beating cardiac cells. This advancement was made possible by employing a new method, Focused Rotary Jet Spinning (FRJS). It enabled the high throughput fabrication of helically aligned fibers with diameters starting from several micrometers to hundreds of nanometers.
Developed at SEAS by Kit Parker’s Disease Biophysics Group, FRJS direct cell alignment, allowing for the formation of controlled tissue-engineered structures. This work may be a breakthrough for organ bio fabrication and brings us closer to our goal of building a person’s heart for transplant. With FRJS, research can accurately recreate those complex structures, forming single and even four-chambered ventricle structures. The beating ventricles mimicked the identical twisting or wringing motion present in human hearts.
Unlike 3D orienting, which gets slower as the features get smaller, FRJS can quickly spin fibers at the single micron scale or about fifty times smaller than a single human hair. This is important when it comes to building a heart from scratch. Take collagen for instance. It would take more than 100 years to 3D print every bit of collagen in the human heart, FRJS can do it in a single day.
Besides bio fabrication, the team also explores other applications for their FRJS platform, such as food packaging. The Harvard Office of Technology Development has protected the intellectual property relating to this project and is exploring commercialization opportunities.









Discussion about this post