What is Meniere’s disease?
Prepare to embark on a journey deep within the intricate chambers of the inner ear, where a perplexing condition known as Meniere’s disease lurks. Like a mischievous enigma, Meniere’s disease surprises its unsuspecting victims with episodes of vertigo, hearing loss, tinnitus, and ear fullness, throwing their lives into disarray. First identified over a century ago by the astute French physician Prosper Meniere, this enigmatic disorder continues to baffle medical experts and captivate the curiosity of those seeking to understand its secrets. In this captivating exploration, we unravel its baffling symptoms, unearthing potential causes, and illuminating the available treatment options. So, fasten your seatbelts as we embark on a thrilling expedition into the realm of Meniere’s disease, where spinning rooms, phantom sounds, and an unquenchable thirst for answers await.
Symptoms of Meniere’s Disease
Meniere’s disease is characterized by recurring episodes of the following symptoms:
- Vertigo:
A hallmark symptom of Meniere’s disease, vertigo is an intense spinning sensation that can last anywhere from a few minutes to several hours. It frequently comes with nausea, vomiting, and trouble balancing.
- Hearing Loss:
Individuals with Meniere’s disease may experience fluctuating hearing loss, which can affect one or both ears. This hearing loss often worsens during episodes of vertigo and may improve between episodes.
- Tinnitus:
Persistent ringing, buzzing, or roaring sounds in the affected ear are common symptoms of Meniere’s disease. This phantom noise can be distressing and may vary in intensity.
- Fullness in the Ear:
Many patients with Meniere’s disease report a sensation of fullness or pressure in the affected ear. This feeling may come and go or persist over time.
Causes and Risk Factors
The exact cause of Meniere’s disease remains unknown, but several factors are believed to contribute to its development.
These factors includes:
- Fluid Imbalance:
The inner ear contains structures responsible for maintaining balance and hearing, including the cochlea and the vestibular system. It is thought that abnormalities in the fluid volume or composition within these structures can disrupt their normal functioning and trigger Meniere’s disease.
- Genetics:
There appears to be a genetic predisposition to Meniere’s disease, as it often runs in families. However, specific genes involved in its development have yet to be identified.
- Autoimmune Factors:
Some researchers speculate that Meniere’s disease may have an autoimmune component, whereby the body’s immune system mistakenly attacks the inner ear, leading to inflammation and subsequent symptoms.
- Other Factors:
Certain lifestyle and environmental factors, such as smoking, stress, and allergies, have been associated with an increased risk of developing Meniere’s disease. However, more research is needed to establish their precise role.
Diagnosis and Treatment
Diagnosing Meniere’s disease can be challenging due to its overlapping symptoms with other conditions. A comprehensive evaluation by an ear, nose, and throat specialist (otolaryngologist) is crucial.
The diagnosis typically involves:
- Medical History and Physical Examination:
The doctor will review the patient’s medical history, including a detailed description of symptoms, and conduct a physical examination to assess hearing, balance, and the inner ear.
- Audiometry and Balance Tests:
Audiometry tests measure hearing ability, while balance tests assess the function of the vestibular system. These tests help identify patterns characteristic of Meniere’s disease.
- Imaging:
In some cases, imaging tests such as magnetic resonance imaging (MRI) may be performed to rule out other potential causes of symptoms.
- Treatment Options:
Although there is no cure for Meniere’s disease, several treatment options can help manage its symptoms and improve quality of life.
These include:
- Medications: Medications such as diuretics, anti-vertigo drugs, and anti-nausea medications can help alleviate symptoms during acute attacks.
- Dietary and Lifestyle Changes: Reducing salt intake and avoiding caffeine and alcohol may help minimize fluid retention and alleviate symptoms. Additionally, managing stress levels through relaxation techniques or counseling can be beneficial.
- Vestibular Rehabilitation: Physical therapy exercises known as vestibular rehabilitation can help improve balance and reduce the frequency and severity of vertigo episodes.
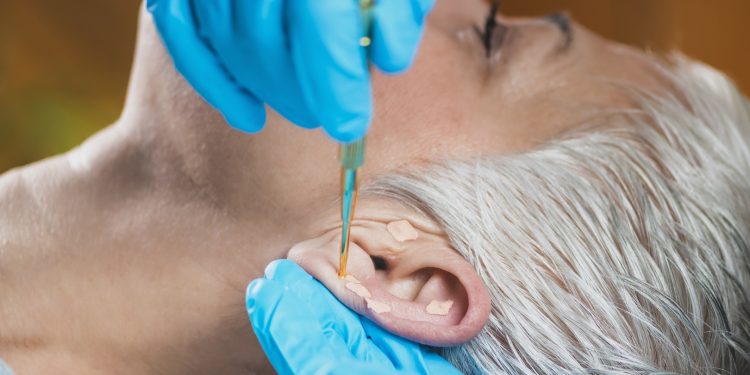
- Injections: In some cases, injections of corticosteroids or gentamicin into the inner ear may be considered to reduce vertigo attacks. However, these treatments carry potential risks and should be discussed thoroughly with a healthcare professional.
- Surgical Options: In severe cases where conservative treatments fail to provide relief, surgical interventions may be considered. These include endolymphatic sac decompression, labyrinthectomy, or vestibular nerve sectioning. These procedures aim to alleviate symptoms by reducing the fluid pressure in the inner ear or disrupting the balance signals.
Coping with Meniere’s Disease
Living with Meniere’s disease can be challenging, but there are strategies that can help individuals cope with the condition. They include:
- Educate Yourself: Understanding the disease, its triggers, and available treatment options can empower individuals to manage their symptoms effectively. Staying informed and seeking support from healthcare professionals and support groups can be valuable.
- Lifestyle Adjustments: Making necessary adjustments in daily life can help minimize symptoms. This includes maintaining a consistent sleep schedule, avoiding triggers such as loud noises or bright lights, and taking breaks during activities that may induce vertigo.
- Assistive Devices: For individuals experiencing hearing loss, hearing aids or assistive listening devices can improve communication and quality of life.
- Emotional Support: Meniere’s disease can have a significant impact on mental health. Seeking emotional support from loved ones or joining support groups can provide reassurance, understanding, and coping strategies.
Conclusion
Meniere’s disease is a complex and chronic condition that affects the inner ear, leading to symptoms such as vertigo, hearing loss, tinnitus, and ear fullness. While its exact cause remains unknown, researchers believe that fluid imbalances, genetics, and autoimmune factors may play a role. Diagnosis requires a comprehensive evaluation, and treatment options focus on managing symptoms and improving quality of life. Through a combination of medication, dietary changes, lifestyle adjustments, and sometimes surgical interventions, individuals with Meniere’s disease can find relief and develop strategies to cope with the challenges posed by this condition. By staying informed, seeking support, and working closely with healthcare professionals, individuals can navigate the journey of Meniere’s disease with resilience and a sense of control.
Reference - https://www.mayoclinic.org/diseases-conditions/menieres-disease/symptoms-causes/syc-20374910 - https://www.nhs.uk/conditions/menieres-disease/









Discussion about this post